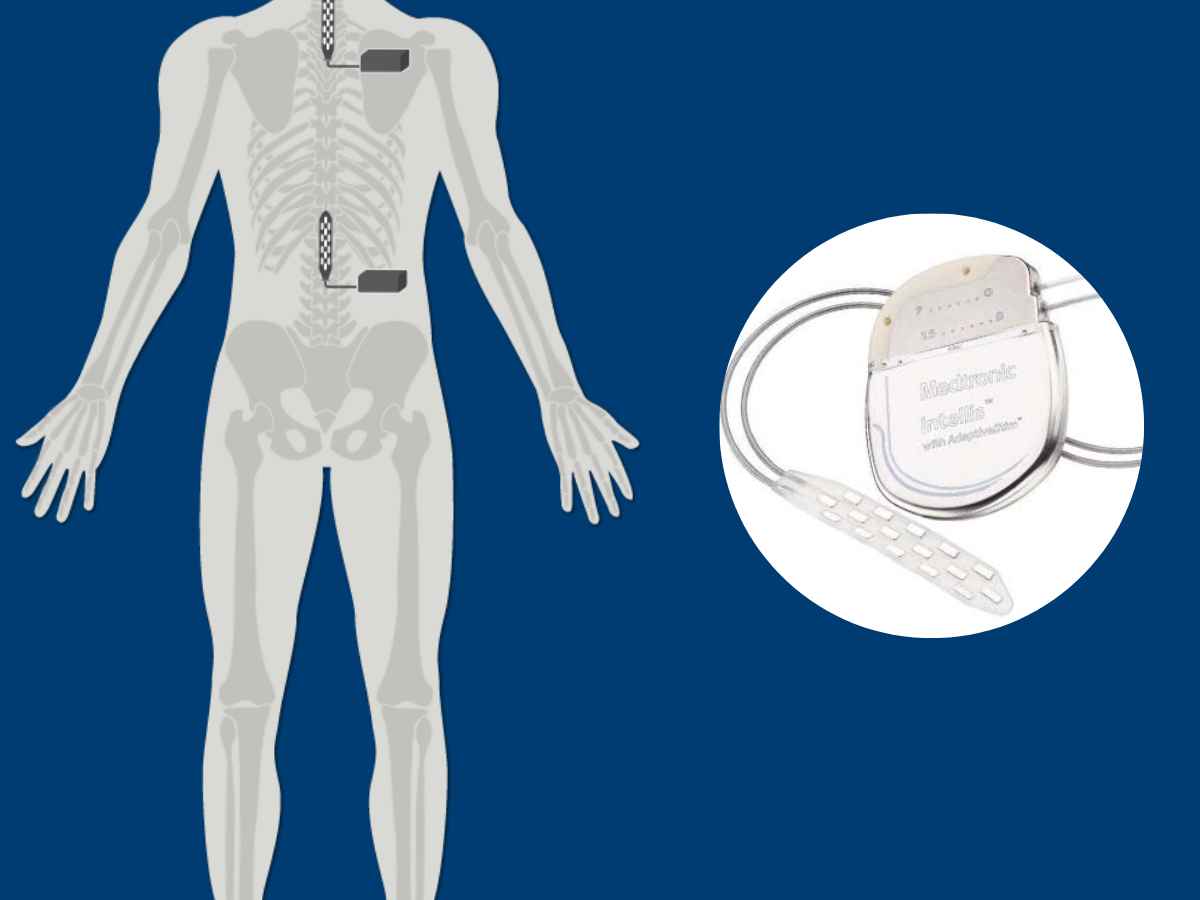
The epidural electrical stimulation implant is one of the most pioneering tools used in contemporary spinal cord injury (SCI) treatment. Chronic SCI is a devastating medical condition and a great majority of the patients face permanent loss of some level of motor, sensory and autonomic functions. A 2018 study in the US showed that over 1 million years of healthy life were lost to SCI over the course of the 44-year study period. For these reasons, demand for a more innovative treatment than traditional physio and occupational therapy-led solutions has been high. The use of the epidural electrical stimulation implant has been extensively clinically trialled and Verita Neuro is the first to offer this solution to the general population. Patients are fitted with one or two implants, based on their specific needs, injury type and injury level.
Significance of the Level of Injury
The level of injury is among the most significant factors that determine the prognosis and the long-term consequences of a severe traumatic spinal injury. Cervical spinal cord injuries lead to the loss of both upper and lower limb functions. Thoracic and lumbar spinal cord injuries, however, only affect the loss of motor function in lower limbs. A majority of patients, regardless of their level of injury, suffer from loss of bowel and bladder functions and sexual functions. Autonomic dysregulation is also common, resulting in impaired blood pressure and temperature regulation.
How the epidural electrical stimulation implant works in SCI treatment
Epidural stimulation for SCI is an advanced form of neuromodulation that targets a specific part of the spinal cord. Each segment of the spinal cord is responsible for a very specific function. For example, the lower cervical spinal cord from C5-T1, called cervical enlargement, is responsible for most of the motor functions in the upper limbs including hands and wrists. On the other hand, the lumbar spinal cord, also called lumbar enlargement, is responsible for our walking ability and contains a huge population of motor neurons, providing nerve supply to muscle groups in the lower limbs. After spinal cord injury, there is a complete or partial disruption of input from the brain, resulting in the inactivation of these segments and rendering them ineffective. The inactivated cervical and lumbar enlargements, however, retain their potential and can be activated using external means of stimulation, such as from an epidural electrical stimulation implant.
Cervical and Lumbar Epidural Stimulation
Statistically, after a severe spinal cord trauma, the lower cervical level is the most common area of injury, which results in partial or complete loss of upper and lower limb functions. This level of injury is by far the most devastating, considering the fact that it significantly affects patients’ abilities to perform activities of daily life (ADLs) resulting in the need for lifelong support.

To improve the patient’s prospects, Verita Neuro offers a highly specialised treatment that combines two epidural electrical stimulation implants, individually targeting upper and lower limb functions. The devices are implanted at the same time, in a relatively short surgery, one at the lower cervical level and another one at the lumbar level. After the procedure each stimulator is calibrated to the relevant limb functions and at a later stage both stimulators are used simultaneously in order to provide comprehensive stimulation to all the muscle groups below the level of injury. This results in patients being able to perform both upper and lower limb functions at the same time.
This combination of two stimulators is a great option for those suffering from cervical spinal cord injuries and had a significant loss of upper limb functions. This may allow them to regain upper limb functions to the extent that they gain more independence in their activities of daily life. Moreover, they can use the lumbar stimulator to stand and walk using upper body support. Long-term use of the lumbar implant also improves bowel and bladder functions and other autonomic functions, including body temperature and blood pressure regulation.
References
- Hall, O. T., McGrath, R. P., Peterson, M. D., Chadd, E. H., DeVivo, M. J., Heinemann, A. W., & Kalpakjian, C. Z. (2019). The Burden of Traumatic Spinal Cord Injury in the United States: Disability-Adjusted Life Years. Archives of physical medicine and rehabilitation, 100(1), 95–100.
- Fuller, D. D., Golder, F. J., Olson, E. B., Jr, & Mitchell, G. S. (2006). Recovery of phrenic activity and ventilation after cervical spinal hemisection in rats. Journal of applied physiology (Bethesda, Md. : 1985), 100(3), 800–806.
- Como, J. J., Sutton, E. R., McCunn, M., Dutton, R. P., Johnson, S. B., Aarabi, B., & Scalea, T. M. (2005). Characterizing the need for mechanical ventilation following cervical spinal cord injury with neurologic deficit. The Journal of trauma, 59(4), 912–916.
- Angeli, C. A. et al. (2018) Recovery of over-ground walking after chronic motor complete spinal cord injury. N. Engl. J. Med. 379, 1244–1250
- Tator, C. H., Minassian, K., & Mushahwar, V. K. (2012). Spinal cord stimulation: therapeutic benefits and movement generation after spinal cord injury. Handbook of clinical neurology, 109, 283–296.