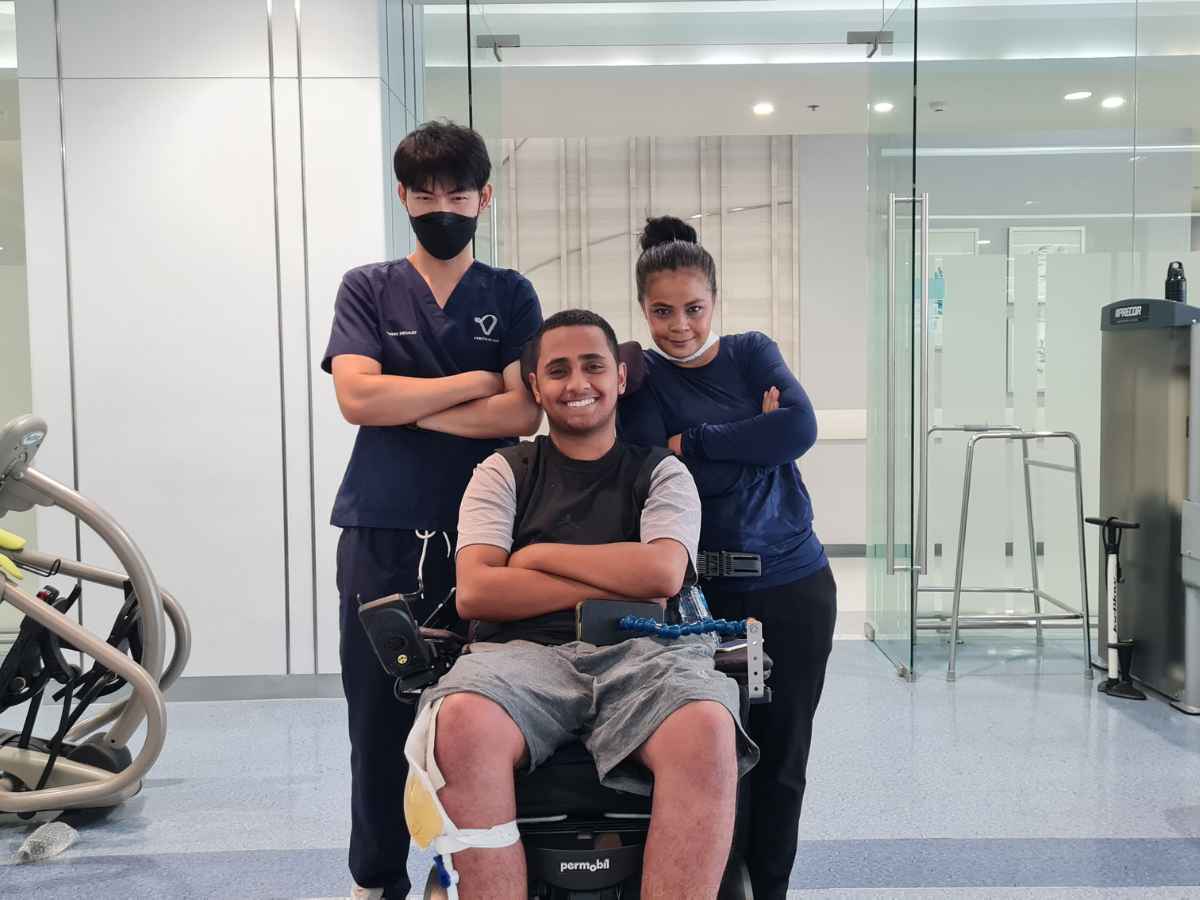
Verita Neuro has always focused on offering patient-centered SCI treatment – collaborating with patients to create the best treatment plan for them. Dylan is a C5-level spinal cord injury patient who came to Verita Neuro in early 2023. His consultation process proved extremely important, allowing him to work with our medical team to create an epidural stimulation treatment program which balanced his goals with what was possible and best for his body. In this conversational interview with Medical Director, Dr. Nasir Majeed and his patient representative, Vea Gaygon, the doctor shares some of the decision-making process and Dylan shares some of his experiences.
Vea: So Dr., I would like to ask, what treatment Dylan eventually received, as I remember from the consultation initially we had different plans. After some collaboration, I believe Dylan pursued lumber stimulation and stem cells and it would be great if you could explain why we suggested this course of action instead of something else.
Dr. Nasir: Of course, so the main concern in Dylan’s case was the loss of lower body motor function. He regained a certain amount of upper body function due to spontaneous recovery after the trauma, extensive physical therapy rehab, and nerve transplant surgeries. So the main concern was loss of motor function in the lower limbs, hence, the main treatment recommendation was to target the lumbar spinal cord. This is the lower part of the spinal cord, which contains motor neurons for the lower body’s motor function. When we looked at Dylan’s MRI scan, we could see the spinal cord was not completely severed – it was damaged, but it was still connected. There were partial signals passing through the injury, going to the lower level and trying to produce some kind of stimulation, trying to produce some movements.
The level of stimulation naturally coming from the brain was not sufficient for the limb to move, so we performed a small surgery to implant a plate of electrodes into the lumbar spinal cord to provide extra stimulation. As a result of the axial stimulation, that part of the spinal cord became super excited and started to produce muscle contractions. I think Dylan can maybe testify that initially, it was random movements but with more training, they are becoming more controllable movements.
This is, of course, the idea behind the treatment, that after the long-term stimulation and long-term rehabilitation, motor control will become better and better over time. This is to the extent where we hope Dylan will have enough strength and control in his body to be able to work with the upper limb support. That’s why I also think his upper body function will be very handy. Because, in my opinion, he has enough strength in his upper body to remain focused on his lower body to improve his lower motor function in the future. So maybe Dylan can also share his experience – I think let’s start with the surgery itself – what does it feel like to go through this kind of procedure?
Dylan: The surgery wasn’t painful at all. Just pretty straightforward. Go in, surgery done, go out, and then start off from there! The only thing that surprised me was when they actually turned on the stimulator straight after the surgery. So that was a big surprise. But after I got used to it became more controllable.
Dr. Nasir: Right, so initially, of course, the patients are not used to the stimulation. So there are sometimes sporadic movements, sporadic sensations. But over time, it becomes more precise, more fine-tuned, and smoother to produce and control those movements.
So Dylan, can you tell us a little bit more about your typical day in your life in the hospital?
Dylan: In the hospital, I do my morning routine, which starts with bowel care obviously. Then around nine o’clock, I go downstairs to do the physical therapy. They walk me through it, they tell me what to do. Now, when they turn on stimulation, I can lift my legs up and move my ankles, up and down. There are two mapping sessions during the day, two hours each and the PT sessions go for one hour a day, six days a week. After PT, they do my upper body. Then in the afternoon, I go back to physical therapy and they give me an e-pacer which helps me stand up and walk! Which I was not able to do before the treatment.

Dr. Nasir: Yes! It’s in its very initial stages and we are just trying to complete the mapping but so far, I believe you have seen some signs of initial recovery! So could you please tell us a bit more about the things you were not able to do before which you can actually do now?
Dylan: I have a bit more sensation in my legs, I can kind of tell when my legs move on their own from the spasms. That’s all I can really think of.
Dr. Nasir: So that’s interesting because the sensation is normally not the area which is being targeted from the stimulation. Those senses normally come from the stem cell treatment, so the improvements in sensation might be attributed to the stem cell treatment. So could you please tell us a little bit more about which muscles you are able to move volitionally when the stimulator is turned on?
Dylan: So when the stimulator is turned on, I can move my feet and my legs up and down. It’s easier for me to lean forward and backward.
Vea: All right, Dr. Nasir, since we were talking about it, can you tell us a bit more about why stem cell treatment is included in the initial treatment and why it is important?
Dr. Nasir: There are two components of the whole treatment plan. The main one is the spinal cord stimulation, which involves a small surgery to implant a neurostimulator in the spine. This provides precise stimulations to different segments of the spinal cord, to move different muscle groups.
The second one is the stem cell treatment. So as we understand, epidural stimulation is excellent when it comes to motor function and autonomic function. When it comes to sensations, it doesn’t really do much on its own, at least not directly. For this reason, we also combine the treatment with stem cell treatments. So stem cell treatment promotes the growth of some spinal fibers at the level of injury, and may help the stimulator to function better. I think this maybe also why it booted the recovery of sensitive function in Dylan’s case and in many other patients. They may need another treatment in the future, but if we can see the partial recovery of sensation even after a single stem cell treatment that is excellent.
Vea: Alright! Dylan, can you tell us how long it took for you to see improvements? What kind of movements did you experience?
Dylan: Probably when I started doing the physical therapy, after the surgery, and after the stem cells, that’s when I started to see more improvement.
Vea: Did you experience any side effects?
Dylan: I think after the first test of the stem cells, I had a little bit of a headache – nothing too major.
Vea: Dr. Nasir, speaking of possible side effects or complications, maybe you can tell us a bit more about it?
Dr. Nasir: Sure. Of course, there are possible risks, which are associated with the surgery itself – a small risk of postoperative infection. The incident rate in our experience is very very low, less than 2%. Then there can be some minor changes in the blood pressure levels because the stimulation may make some changes in the sympathetic pathways, the part of the nervous system responsible for blood pressure regulation. So the stimulation to those specific areas may produce some temporary or mild changes in some patients, particularly if the injury is at a higher level. From the stem cell treatment, there is a small risk of headache, fever, back pain and sometimes nerve pain in the legs.
We have a question for Dylan – when was your accident?
Dylan: January 26? Pretty sure, 2022.
Dr. Nasir: We call the first 2 years after injury a golden period for some potential recovery. So basically, in the first two years, there are important pathophysiological changes in the spinal cord, where our body is trying to replace the diseased or injured tissue with scar tissue. This is a natural defensive mechanism from our body, but it is also devastating for any potential future recovery. Once the area is completely sealed off with scar tissue, it becomes extremely difficult to regenerate or regrow the tissue. So that 2 years is the period where, if possible, patients should receive the treatment to maximize the chances of recovery. This is also important for stem cell treatment, because stem cells may be able to reduce the inflammation to keep the window period for recovery open for a longer period of time. But having said that, we also have had patients who are many years after the injury, basically, sometimes 25, sometimes even 30 years. The recovery may take longer periods of time, at least for the motor function recovery, but it’s possible. But, overall, the sooner, the better is my general answer.
Vea: All right! There is a question Dylan, did you see any improvements or what kinds of improvements are you seeing with bowel and bladder functions, if any, at this point?
Dylan: I haven’t really seen any improvement yet.
Vea: Doctor in terms of bowel and bladder function, do we see it later?
Dr Nasir: Normally, it comes gradually over a period of time. We have to continue to use the stimulation, to provide long-term consistent stimulation to the sacral spinal cord, which is slightly below the lumbar spinal cord. It doesn’t receive direct stimulation, but indirect stimulation over longer periods of time. This can regulate autonomic activities at the cellular level, which can improve bladder and bowel function. Stem cell treatment can also play a small role in this area.
For the bladder function, there are three components of the bladder function. One is the sensory functions. The other is autonomic and the third is somatic muscle function. These three components of the nervous system need to come together to produce a significant recovery. So we have seen some partial recovery in the bladder function, bladder sensation, and also partial recovery in the patient’s ability to control the bladder and push the urine out. But I think a full recovery is not something which we really expect – a partial recovery is possible. That too also comes after some time, it doesn’t happen immediately.
Dylan, can you tell us a little bit more what your plans are when you go back to Australia?
Dylan: I’ll probably take next week off, just get back into Australia time. Then maybe in the next fortnight, I’ll probably start going back to physio, four days a week. I usually go for one hour, but luckily, at home, just when I’m with my mates or Dad, or my uncle, I’ll do what I usually do with physical therapists.
Vea: It sounds like to me you have seen some improvements – what do you think is the most significant change that has happened to you?
Dylan: The most significant was being able to move my leg. I started walking training, I think maybe week two, and ever since then, it’s improved significantly.
I’ve seen changes in my seating balance. It’s not 100% there but with the stimulation on, that helps a lot. I’m just picking myself back up, bringing myself forward.
Vea: OK you’re coming to the end of your stay. What did you like most during your stay?
Dylan: The physical therapists are very welcoming and very encouraging, as well as the doctors, everyone’s very up-to-date. The mappers definitely know what they’re doing, they’re very supportive, very encouraging. They showed me different ways of how to lift my legs up, and how to move around.

Vea: Do you have a message for people who are watching and considering the treatment?
Dylan: Do it, stay mad about it, be consistent, work hard and believe in yourself.
The above is not a verbatim transcript of Dylan’s interview. Some comments have been altered or re-arranged in order to improve the reading flow. If you would like to hear the full webinar, you can view it on our youtube channel here.